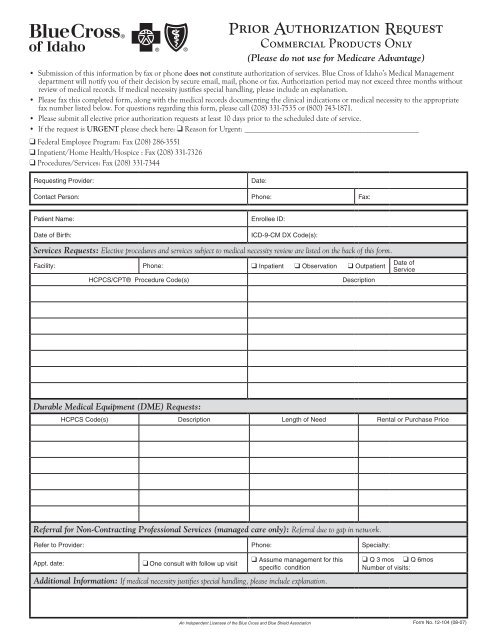

Protections for Enrollees in MA Plan Transitions While these requirements aren't new, CMS is reminding MA plans that they need to follow them. The final rule limits MA plans’ ability to employ prior authorization and utilization management policies for reasons beyond confirming the presence of diagnoses or other medical criteria, or to ensure that a service or item is medically necessary. 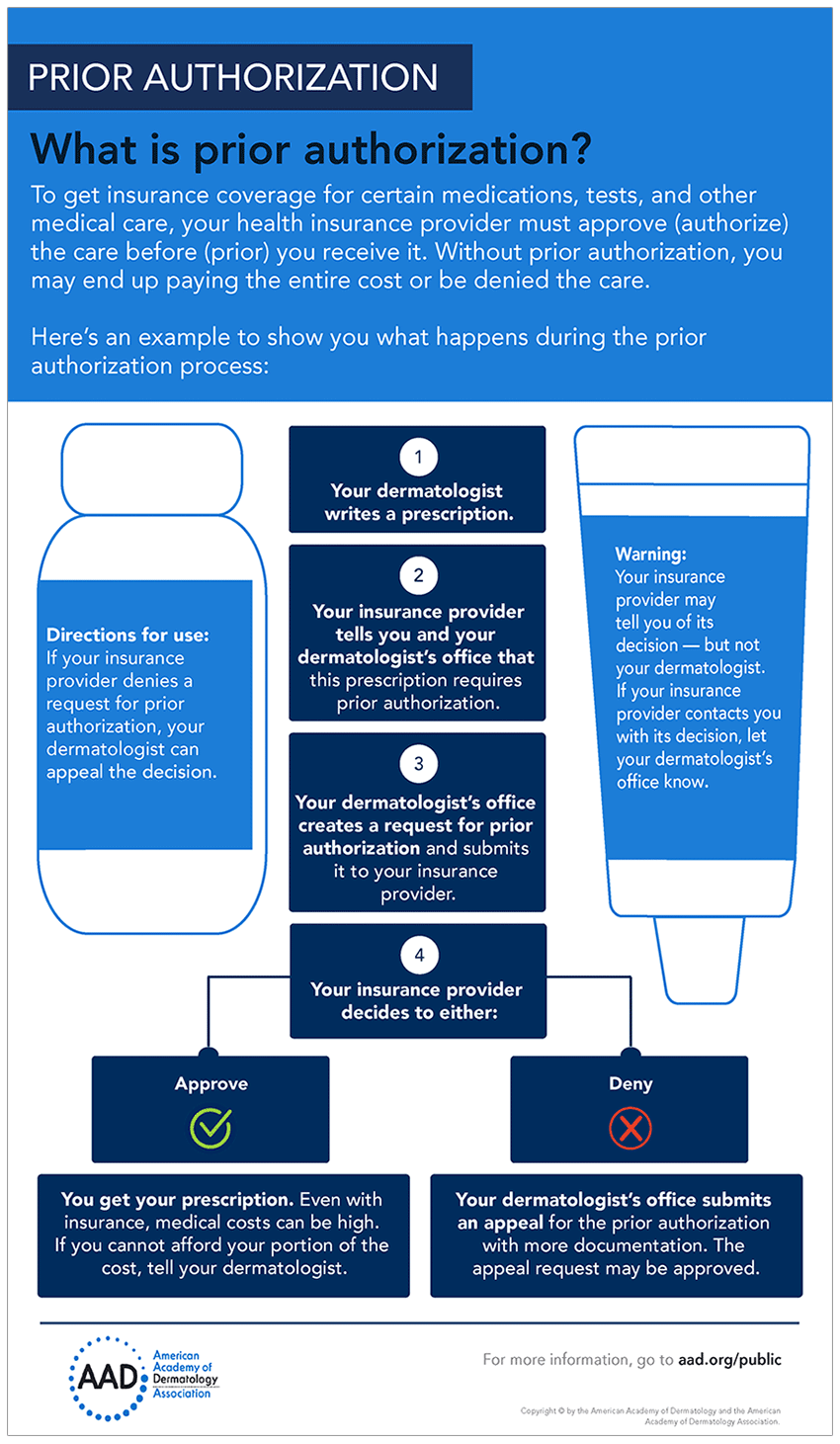
These changes were made to the existing minimum continuity and coordination-of-care requirements. In a significant shift that will place greater weight on clinician judgment, an approval of a prior authorization request for a course of treatment now must be valid for as long as medically necessary to avoid disruptions in care in accordance with applicable coverage criteria, the patient's medical history, and the treating provider's recommendation. Prior Authorization Approvals to Remain in Effect for as Long as Necessary According to a CMS fact sheet, the intent is to ensure that MA enrollees receive the same services and items as beneficiaries in the Medicare fee-for-service program. Taken as a whole, the prior authorization-related changes in the final rule are aimed at ensuring MA plans don't apply requirements that disrupt care. Prior Authorization Versus Preserving Continuity of Care Among the provisions of the 2024 MA final rule: limits on the application of prior authorization, assurances that a prior authorization approval remains valid as long as medically necessary, and accommodations for patients in transition from one MA plan to another. Centers for Medicare & Medicaid Services has put up additional guardrails on the use of prior authorization in Medicare Advantage plans. In a win for APTA and other organizations fighting to reduce administrative burden, the U.S.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
